|
Acute
septic arthritis affects all age groups.
It is caused by haematogenous spread of a bacterial organism,
or by a penetrating injury. The joint is swollen and painful to move.
Treatment is by arthrotomy and irrigation, appropriate antibiotic
therapy, splints and physiotherapy.
SUMMARY
Septic
arthritis is usually a monoarthritis. It is a febrile condition;
joints affected have painful motion and an effusion.
The most usual causative
organism is Staphylococcus areus,
but the intracellular cocci such as pneumo or gonococcus are common.
In neonates and infants younger than 6 months, S aureus and gram-negative
anaerobes comprise the majority of infections.
Treatment is by antibiotics and effective irrigation of the joint
by open arthrotomy. Postoperative physiotherapy and mobilisation of
the joint
is necessary, while splinting prevents contractures.
Early treatment may prevent severe complications such as dislocation,
acvascular necrosis and late osteoarthritis.
Etiology: Most septic arthritis cases are caused
by Staphylococcus aureus and streptococci. In neonates and infants
younger than 6 months, S aureus and gram-negative anaerobes comprise
the majority of infections. Haemophilus influenzae is commonly seen
in neonates and children up to 2 years age (in South Africa, although
in many developed lands the incidence due to this organism, has dramatically
decreased due to widespread use of the vaccine). After 2 years S Aureus
(as in the case of acute osteomyelitis)is the main causative organism.
In the sexually active patient, Neisseria gonorhoeae is a common culprit.
DIAGNOSIS and MANAGEMENT PROTOCOL
The patient complains of spontaneous onset of pain in a joint. Episodes
of penetrating trauma e.g. knife wound or thorn must be enquired
about, as well as previous febrile illnesses, osteomyelitis and
sexually transmitted diseases.
The patient is systemically ill. Superficial joints have an obvious
effusion and are warm. The is painful on movement with pain on
less than 5 degrees joint movement being characteristic. Children
usually present with an acute
febrile illness and a swollen painful joint. The exception is the
immunologically suppressed patient, the elderly, and neonates,
who may produce minimal clinical signs. In the neonate (especially when
in a temperature controlled environment, such as an incubator) Pseudo
paralysis or failure to spontaneously move a limb, is often
the only clue to septic arthritis.
Special Investigations:
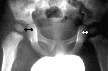 X-rays - may show widening of the joint space, indicating an
effusion.
X-rays - may show widening of the joint space, indicating an
effusion.
This X-ray shows an effusion
- widening of the right joint space
Haematology - ESR
and white cell count raised
Blood culture - recommended in
children who present with a septicaemia- (80% Specificity)
Joint aspiration - (may be done as a diagnostic test, but is
not an effective treatment modality. It only recommended for superficial
joints,
where diagnosis is in doubt)
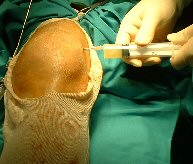 |
Aspiration of knee. Observe aseptic precautions
- insert a needle into the joint by placing it under the patella,
either medially, or laterally. |
Appearance of synovial fluid in septic arthritis. Pus
colored fluid (yellow or green), with WBC count of >100 000 cells
/mm^3,
The other condition that gives high white cell counts is crystal synovitis
(do polarised microscopy, and check the serum uric acid for elevated
levels, if gout is suspected)
Synoial glucose level: Low synovial
glucose level (40 mg/dl or less than half the serum level) is suspicious
of a pyogenic joint infection.
Prevention:
Explore and debride all deep wounds in the region of a joint.
Neglect of this principle, with mere suture of a penetrating wound near
any joint will likely to result in septic arthritis. Wounds particularly
at risk are those near the knee and the knuckles. (street fighter ,with
tooth penetrating. MP joint).
Treatment:
The joint needs to be thoroughly irrigated and appropriate antibiotic
therapy started. Aspiration of a superficial joint is acceptable for
diagnostic purposes, but will not rid a joint of all pus. Deep joints
such as the hip are difficult to aspirate and failure to obtain pus
may simply be because of faulty technique.
An open arthrotomy is recommended in most cases. Arthroscopy is also
an effective method of thoroughly rinsing out a joint.
It allows, usually inaccessible regions of the joint, to be reached
for lavage. High volume irrigation is possible through the arthroscope,
allowing inaccessible parts of the joint can be visualised. Repeated
needle aspirations and irrigation, is another modality, but is
not as effective as the above methods, and should be reserved for
superficial joints, in patients with high anaesthetic risk. A single
aspiration will not be effective in draining a joint of thick pus and
the procedure needs to be repeated daily.
Preoperative
preparation will include an intravenous drip and adequate
rehydration. Blood transfusion may be needed, especially cases
of Staphylococcal septicaemia ( haemolysin). The patient may have other
concomitant infections such as bronchopneumonia, meningitis (meningococcus)
or osteomyelitis. These will also have to be addressed as they affect
the anaesthetic risk. Under full or regional anesthesia, the joint is
opened via an appropriate incision that gives good exposure to
the joint.
After incision of the capsule pus swabs are taken of the synovial fluid
for microscopy and culture. The joint is irrigated via a syringe and
all pus is washed out. If the infection seems chronic, or the symptoms
atypical, a synovial biopsy is taken. (Histology, MC&S for possible
Tuberculosis). In children symptoms and signs of acute osteomyelitis
are very similar.
Because of the possibility of concomitant, or misdiagnosed acute septic
osteomyelitis a drill hole in the adjacent metaphysis maybe warranted
in patients with open physes, especially if the joint does not
contain obvious pus.
The synovuim is sutured. If significant pus was found , the wound
is left open for later secondary suture,
otherwise, use a suction drain and close the wound.
Postoperative
Care:
Antibiotics are given intravenously until the temperature is
normal, followed by oral antibiotics. Organisms responsible are
Staphylococcus
(especially in children), The intracellular cocci
e.g. Meningococcus and Gonococcus, in sexually active patients are not
infrequent.
In the immune compromised patient, atypical organisms, such as fungal
may be encountered. Clinical judgment as to appropriate antibiotic therapy,
must be used in view of the above variety of causative organisms.
E.g. a child. will probably have a Staphylococcal infection and
Cloxacillin and Erythromycin would give good cover before pus swab results
could give better guidance.
Physiotherapy - most joints
need motion rather than immobilisation.
If the cartilage seems still viable, mobilise the joint with a
continuous passive motion machine, if available, or regular active
and passive physiotherapy. To prevent contractures , apply traction
or splints while the patient is not exercising. Appropriate for
the hip would be skin traction and for the ankle a plaster back
slab.
In advanced or neglected septic arthritis there may be little hope
of later joint function. It is then appropriate to permanently immobilise
the joint in a functional position, so that the joint can ankylose.
Here a spicka cast for a hip or full length cast for a knee may be applied.
Prevention and management of complications:
Advanced arthritis can result in many serious complications. If
the effusion recurs repeated explorations and debridements of the
joint might be necessary. Suspect tuberculosis if the arthritis
does not respond to this regime and take a biopsy.
E.g. Arthritis of a child's hip can result in:
Complications of Septic
Arthritis Hip in a child
(a) Dislocation
Is often seen in the hip due to the overdistended capsule. Traumatic
dislocation of a child's hip is rare, consider sepsis as one of the
causes if a hip dislocation is seen in the young child.
(b) Osteomyelitis of the femur
(c) Avascular necrosis femur head
(d) Ankylosis
(e) Late osteoarthritis
|
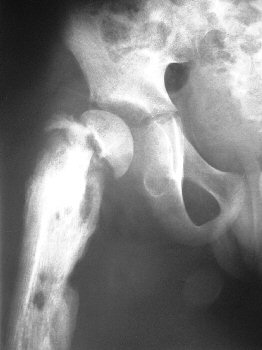
The photo shows the late complications
of septic arthritis.
Note the chronic osteomyelitis of the femur shaft. The femoral
neck has fractured and the femoral head is loose and avascular.
There is widening of the joint space. The effect of the absent
growth plate will be measured in later years as the femur progressively
shortens relative to the normal side. |
Postoperative Course
The ESR should return to normal within a few weeks.
A septic joint may need more than one trip to theater for irrigation.
If the arthritis does not clear up rapidly on the above treatment,
suspect tuberculosis. Take synovial specimens for histology in all acute
arthritides, which do not respond to antibiotics.
TB is one of the few causes of arthritis that can be diagnosed
on light microscopy.
Further Reading
1. Nord K. D. Evaluation of treatment modalities
for septic arthritis.
JBJS Vol 77 A, No 2, February 1995, pp 258-265 http://www.ejbjs.org/cgi/content/abstract/77/2/258
2. Peltola Reduced incidence of Septic
Arthritis in children by Haempophillis influensae
Type B vaccination: Implications for treatment J Bone Joint Surg [Br]
1998; 80-B; 471-3 http://dx.doi.org/10.1302/0301-620x.80b3.8296
3. Kang SN, Sanghera T, Mangwani J, Paterson JMH,
Ramachandran M. The management of septic
arthritis in children: SYSTEMATIC REVIEW OF THE ENGLISH LANGUAGE
LITERATURE. J Bone Joint Surg Br 2009;91-B:1127-33.
4. JM Nel, A Visser, HF Visser, k Goller, R Goller:
Adult septic arthritis in a tertiary setting: A Retrospective analysis:
SA Orthopaedic Journa 2009l; Vol 8 No 3: 53-58
|
 X-rays - may show widening of the joint space, indicating an
effusion.
X-rays - may show widening of the joint space, indicating an
effusion.
