Robert Jones Bandage
This is useful for injuries that have a danger of swelling e.g. Ligamentous damage
to the knee.
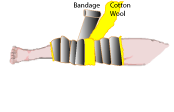 |
| Robert Jones Bandage |
It consists of three alternate layers of cotton wool and crepe bandage.
The bulky Robert Jones Pressure bandage minimises further swelling and
it affords some immobilization.
If necessary the bandage can be made more rigid
by application of plaster slabs to the sides.
These are secured by another layer of bandage.
Plaster of Paris
The chemical composition is Calcium Sulphate on a fabric mesh
The plaster sets by adding water of hydration
(CaSO4, 2 H2O) + heat = (CaSO4, ˝ H2O) + 1.5 H2O)
Gypsum was discovered 9000 years ago in Syria
This causes an exothermic reaction.
This increase in temperature can burn the skin
if the reaction is too fast e.g. use of hot water or, if the patient
places the cast near a radiator.
Reduction
The sooner the reduction of a fracture is attempted the better, because swelling
of the extremity tends to increase for 6 to 12 hours after the injury.
Before embarking on the manipulative reduction,
adequate x-ray films must be obtained to determine what the objectives
of the manipulation are to be or if, indeed, a reduction is necessary.
Perkins stated that closed reduction is contraindicated when:
Contraindications for closed reduction
1. There is no significant displacement.
2. The displacement is of little concern (e.g., humeral shaft).
3. No reduction is possible (e.g., comminuted fracture of the head
and neck of humerus).
4. The reduction, if gained, cannot be held (e.g., compression fracture
of the vertebral body).
5. The fracture has been produced by a traction force (e.g., displaced
fracture of the patella).
To achieve a reduction, the following steps usually are advised:
(1) apply traction in the long axis of the limb;
(2) reverse the mechanism that produced the fracture; and
(3) align the fragment that can be controlled with the one that cannot.
Immobilization
Once a satisfactory reduction has been achieved, it must then be maintained until primary union has taken place. Immobilization may be provided by a cast, continuous traction, or some form of splint.
Principles of plaster technique
- Practice the reduction before cast is applied
- Pad all fresh fractures - use wool such as "Velband"
- Apply this padding evenly
- Water must be slightly warm
- Work the layers to get laminations to bind
- Never flex a joint after POP is applied - hold it flexed beforehand
- Three pressure points are needed to keep reduction
- These pressure points must not cross a joint
Further
information on basic plaster technique can be found in this document.
Follow up of a cast
- Immediate post-reduction X Rays
- Split plaster if any danger of swelling
- Elevate limb
- Circulation check 24 hours later
Swelling is maximal the first 48 hours and then subsides. Once the patient
discharged from your casualty, he must be seen and the reduction checked
within a week. If necessary the cast can be replaced at this stage.
A new reduction may be needed if the fracture has displaced at this
stage. After a week some fractures e.g. growth plate injuries become
increasingly difficult to manipulate.
