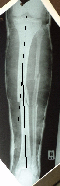
Fractures of the tibial shaft are common. Due to the subcutaneous nature of the distal part of the anterior shaft, these fractures are often open.
Management: Shaft fracturesTibial fractures are often due to high velocity trauma. Remember to look for other injuries, including chest and abdominal trauma. Check for other fractures and dislocations, especially of the ipsilateral knee and hip.
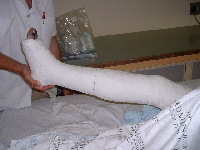
ExaminationCheck for diatal pulses. Make sure there is no nerve fallout, especially the peroneal nerve (drop foot). Any wounds present alert you to te presence of an open fracture. Wounds near the fracture need exploration in theater. Here the decision can be made as to whether the wound communicated with the fracture or not. Closed FracturesConservative Treatment Stable and minimally displaced fractures can be treated conservatively by reduction and an above knee cast. If the fracture is minimally displaced a general anesthetic may not be necessary. Use a general anesthetic if there is overlapping of bones, or difficulty is expected.
Take a check X Ray to confirm your reduction. Keep the patient overnight, or instruct him to return for a circulation check the following day. The next follow up can be at one or two weeks. Here the plaster is checked. X rays are taken in the cast. If there is angulation wedging can be done of the cast. If there is unacceptable loss of length this method will fail and a remanipulation or possibly open reduction and internal fixation is required. Wedging a plaster. Measure the angulation on the x ray (leg still in plaster). Extend a line at right angles to the shaft at both sides of the fracture onto the image of the plaster. This will be equivalent to the gap to open. The plaster is sawed open at the fracture level - keep a intact hinge open at the opposite side. hinge the limb into alignment by opening the gap in he plaster and holding it with a wooden block. Check X rays are taken. Once the desired result is achieved repair the defect with plaster bandage.
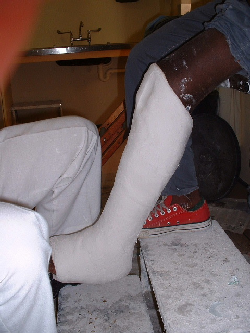
Once the doctor is satisfied with alignment, the patient is followed up as an outpatient. Once the fracture starts stabilising after the initial few weeks he is seen monthly. The plaster cast is kept on with only replacements when seen at the clinic. At this stage X rays can be taken out of plaster, as callus formation is better assessed on X ray without a cast. For mid shaft or lower fractures a patellar bearing cast often speeds up union.
|
|||||||||||||||||