Open Reduction
Recently there has been a swing towards intramedullary pinning of the tibia. The procedure has a low sepsis rate and pin breakages are rare. Any closed unstable fracture of the shaft (large butterfly segment or comminution) can be considered candidate for this method. It is difficult to successfully plate a tibia shaft as there is a high rate of sepsis due to its poor distal blood supply, and the proximity of the skin to the bone lets in sepsis.
Open Fractures
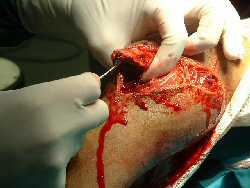
Play animation on how to debride an open fracture (1 min40 sec) Click to play: Debridement Video Tibial fractures are often open due to most of the anterior border of the shaft being subcutaneous. The wound must be inspected in the trauma ward and then covered with a sterile dressing. A broad spectrum antibiotic is given (first generation cephalosporin plus amiloglycocide if very contaminated) Prophylaxis against tetanus is also necessary.
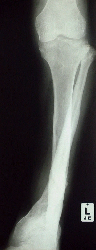
In theater the leg is scrubbed before it is draped. The wound is incised to a larger size if it is too small for access. All dead tissue is excised. Viable muscle will bleed, and should contract if pinched with a forceps - if it does not it needs excision. Preserve nerve tissue and suture if transected. Vessels may need repair at his stage. Lose pieces of bone ( no muscle attachments) are discarded. Leave the wound open for secondary suture later. take tissue and pus swabs for areobic and anaerobic culture) The wound needs irrigation with copious water (10 litres or more). A pulsed lavage system is invaluable in getting fine contaminants out of the tissue. If there is a large soft (Gustillo 3b type or more ) tissue defect consult a plastic surgeon regarding a primary flap to close the defect. The limb is stablised - use an exfix if the wound is large or will need attention later (skin graft etc.) If the wound is small and easily closable a paster cast may be necessary. Open reduction is not recommended at this primary debridement. It may be done at a later stage (48 hr.+) in the less contaminated fracture (below Gustillo 3B). A second debridement at 48 hours is recommended in all contaminated cases. Here further non viable tissue is identified and removed. Wounds may be sutured at this stage if the wounds appear clean. Delayed and Non UnionThe tibia should begin to show signs of callus formation on X rays
from six weeks onwards. The fracture becomes less mobile when stressed
and the pain diminishes. If the tibia does not show signs of union
or does not progress as expected delayed union may be diagnosed.
Treatment of delayed union needs to address the cause. Conservative
treatment such as a dynamic cast (patellar tendon bearing cast) may
stimulate union. If this fails, surgical measures are necessary. If
sepsis is the cause a sequestrectomy of the fracture area is needed.
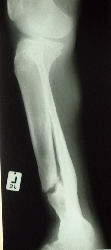
If there is abundant callus but none bridges the gap (hypertrophic delayed
union -"Elephant's foot" type) more stability is called for.
An open reduction and internal fixation may be needed. |
||||||||||||

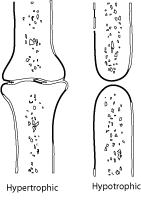 Hypotrophic
delayed unions ( where there is little callus) are due to vascular reasons
(e.g.severe stripping of soft tissue in an open fracture) Here a bone
graft as well as further stabilisation (ORIF or Exfix) will be needed.
Mal alignment is a potent cause of non or delayed union, as there are
shear and angulatory forces tearing apart all attempts by capillaries
to bridge the fracture gap. In this case a realignment procedure with
fixation by exfix, or intramedullary pin is called for.
Hypotrophic
delayed unions ( where there is little callus) are due to vascular reasons
(e.g.severe stripping of soft tissue in an open fracture) Here a bone
graft as well as further stabilisation (ORIF or Exfix) will be needed.
Mal alignment is a potent cause of non or delayed union, as there are
shear and angulatory forces tearing apart all attempts by capillaries
to bridge the fracture gap. In this case a realignment procedure with
fixation by exfix, or intramedullary pin is called for.