Dr. A.A.Rawoot Tygerberg Hospital 18 March 2009
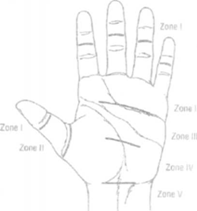
Anatomy Zone 1: FDS insertion to FDP insertion Zone 2: Zone 1 to proximal part of Al pulley Zone 3: Zone 2 to distal edge of flexor retinaculu Zone 4: Within carpal tunnel
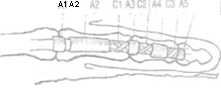
Thumb T2: Zone 1 to distal part Al pulley Thumb T3: Zone 2 to carpal tunnel Pulleys 5 Annular, 3 Cruciform Fibrous annular pulleys prevent bowstringing A2 and A4 most important Cruciate pulleys are thin and provide flexibility Tendon repairs through C l and C2
Extra-synovial : forearm - palm - paratenon Synovial : Carpel Tunnel & digital flexor sheath - vincular arterial system - diffusion from synovial fluid - additional supply from distal oseous attachments
Watershed areas (Lundborg) : FDS under the A2 pulley FDP under the A2 pulley and A4 pulley
Intrinsic repair response Lundborg and Rank (1978) - intra-synovial flexor tendons initiate intrinsic repair response after tendon transection Gelberman et al (1980s) - studied effect of early digital mobilization following flexor tendon repair in zone 2 - immobilized: j linear tendon excursion formation of peritendinous adhesions (extrinsic tendon repair) - mobilized: | linear tendon excursion (intrinsic repair response) Early restoration of gliding surface by day 10
Stages: Inflammatory phase (0-14 days) Reparative phase (2-6 weeks): Remodeling phase (> 6 weeks): Inflammatory phase (0 - 14 days): Fibrin clot forms at repair site Macrophage and leukocyte migration Phagocytosis Growth factors ( bFGF) peak Cells from epitenon proliferate and migrate to repair site Gliding surface restored Strength of repair is related to strength of suture
Reparative phase (2-6 weeks): Intense collagen production - mostly type 1 Gradually orient themselves along the axis of tensile forces Epitenon cellular ingrowth fills repair site gap Neovascularization Strength increases at 2 weeks post-op Repair site strength still principally related to the suture strength & material
Remodeling phase (> 6 weeks): Collagen fibers smooth and uniform Collagen fibers are remodeling to be oriented parallel to the longitudinal axis Increased repair site strength
Extrinsic repair response Dominated in the immobilization group By 10 days after repair, the in-growth of peripheral adhesions dominated the repair site
Surgical principles Operating room, loupe magnification GA or regional anaesthesia Tomiquet Meticulous tissue handling (Bunnell) Bruner type (zigzag) or midlateral incision, incorporate original lacerations Identify & protect neurovascular bundles Avoid devascularization of skin flaps Locating tendon ends: - haemorrhage within tendon sheath - 'milking' proximal to distal - grasping exposed interior substance of tendon stump with fine toothed forceps - pre-op ultrasound Avoid blind passage of instruments into tendon sheath - promote intrasynovial adhesions If proximal tendon is retracted & inaccessible, retrieve by distal - proximal passage of small feeding catheter 20G needle placed l-2cm prox + distal to transected ends to stabilize ends for repair Protect annular pulleys, especially A2 and A4 Do repairs through C1 and C2 Reconstruct sheath where possible
Surgical technique
No man's land Attributed to Bunnell 1934 Zone 2 Discouraged primary repair in this zone The preferred treatment was free tendon grafting Kleinert reported excellent results with primary suturing in 1967 Then it was believed that only FDP should be repaired in zone 2. Now, in experienced hands, it is believed best to repair both FDS and FDP (FDS first)
Suturing material Braided polyester fiber 3/0 or 4/0 most popular Flexibility & ease of handling Minimal mechanical trauma to tendon Allow early digital mobilization
Repair methods Core sutures: greatest tensile strength - multiple sites of tendon interaction - Kessler/ modified Kessler, Bunnell - newer - Tajima, Strickland At least 4 strand core suture Dorsal placement of core suture Locking better than grasping Knot placement does not have an effect on tensile strength but placement away from the repair J, tendon glide
Multistrand positives: - Less gap formation - Less tendon ruptures Multistrand negatives: - Technically more difficult - Tendon thicker - Increased gliding resistance
Epitendinous sutures | repair site bulk 1 tensile strength Bite of 25% of diameter of tendon Obliquely lacerated tendons Change from modified Kessler (grasping) repair to locking Kessler repair Lengthen the longitudinal strands
Partial tendon lacerations General consensus that lacerations of less than 60% of the tendon substance should not be repaired Potential complications: - triggering - entrapment - late rupture Beveled edge can be trimmed
Annular pulley injuries A2 and A4 pulleys should be repaired or reconstructed if they are deficient Reconstruction can be done by using a free tendon graft or part of the extensor retinaculum
Rehabilitation Surgical technique and quality of repair likely attributes to only 50% of end result success Different rehab protocols - no method guarantees successful outcome in all pts
Early moblization following tendon repair: - stimulates tendon healing - minimises adhesions Controlled motion of healing tendon - improves tensile strength - improves gliding Tendon excursion of 3 - 5 mm required to prevent firm adhesions ( Duran & Houser) Rehabilitation should be individualized: 1. Type of injury 2 Quality of repair 3. Compliance of patient 4. Patient's insight
Rehabilitation - Methods Early Passive Motion Fingers splinted in flexion - rubber band traction Pt instructed to extend fingers actively for 5sec Repeated 10 X / hour Bands left unattached at night & during alternating periods - prevents flexion contractures of IPJ's Warn pts against passive extension of wrist & fingers
Dorsal splint: - wrist: approximately 20 degrees flexion - MCPJ's: approximately 40 - 70 degrees flexion - IPJ's: full extension
Negatives: -Significant loss of PIP J extension -Poor mobiliser of the DIP joint if used without distal palmar bar
Early Active motion Dependant on - strong repair - early referral to OT - pt comprehension & compliance Wait 3-5 days - avoid fresh bleed & adhesions Dorsal blocking splint Initial passive flexion & extension - overcome stiffness 'place & hold' exercises: finger placed in flexion & held for 5sec Gentle active flexion +/- 14 days post op
Rehab - wk 5-6 Splint removed for hand wash, lotion or hand cream, scar tissue massage Active movement with minimal resistance Splint remoulded - more wrist ext Paraffin wax or U/S - reduce joint stiffness Tendon gliding exercises Rehab - wk 7 - 12 Dorsal splint worn at night Activities against resistance introduced Return to light duty Return to normal duty by wk 12 No contact sport for another 4 wks
Complications of Flexor tendon repair Gap formation - due to: - breakage of suture material - inadequate suture method - poor immobilization - excessive prox muscle pull (Lindsay & Thompson) > 3 mm: No significant repair-site tensile strength increase between 3-6 weeks > 3 mm: Gap filled with fibrosis > 3 mm: Gap progressively increased in size till tendon eventually ruptured Less gap formation with multistrand, multigrasp suture methods - 4 strands being optimal Tendon rupture 50% because of pt non-compliance May present like infection Prompt re-exploration and repair
Infection
Flexion contractures Prompt recognition NB: Extend PIP's and DIP's fully and regularly during exercises Addition of palmer bar to dorsal splint
Bowstringing Triggering
Extensor Tendon Rehab Dynamic Splinting with early passive motion - D5 post-op - dorsal dynamic extension splint ( wrist 40-45 ext, MCPJ rests at 0 ) + palmar block - allows controlled flex of MCPJ 0-30 - achieve gliding of repaired tendon - passive flex of IPJ's through FROM within splint - 3 - 4 wks post-op palmar block removed - T MCPJ flexion & tendon excursion allowed - initially fingers ext with short lever arm (IPJ's flexed) - wrist in slight flex ( wrist flex synergistic with finger ext)
Passive splinting with early active motion - D3 - 5 post-op, hand placed in volar splint ( wrist 40-45 ext, MCPJ 20-30 flex ) - 'place & hold' exercises in the splint - progress to active ext of MCPJ from 30-0 - splint worn for 4 wks then shortened Either treatment regime may still lead to ext tendon adhesions over MC Early oedema control, digital scar massage, early motion prevent adhesions |
Tendon Injury to the Hand
Department of Orthopaedic Surgery - University Stellenbosch
| Flexor and extensor injuries to the hand |