Fractures of the distal femur shaft are more difficult to treat conservatively. The gastrocnemius muscle crosses the knee and pulls the distal fragment into flexion thus causing a posterior angulation.
 If treated conservatively a two Denham pin method is often necessary.
One pin is placed into the proximal tibia and the other is inserted into
the distal femur. The Femoral pin's line of traction is superior and the
Tibial pin is pulled horizontally.
If treated conservatively a two Denham pin method is often necessary.
One pin is placed into the proximal tibia and the other is inserted into
the distal femur. The Femoral pin's line of traction is superior and the
Tibial pin is pulled horizontally.In all cases the knee must be in flexion (about 60 degrees)to relax the pull of the gastrocnemei.
Supracondylar and Intracondylar fractures
A fracture that occurs just above the femoral condyles often has an intracondylar extension and one or both the condyles may be loose.
 |
| Supracondylar femoral fracture with no intracondylar extension |
Displaced fractures that are intracondylar always need internal fixation. If unicondylar the fracture is anatomically reduced and fixed to the intact condyle with screws. If both condyles are loose a blade plate or a buttress plate (or locked plate) and screws will be necessary. Plates and screws are inserted on the lateral side as this side of the femur is in tension and can tolerate a fixation device longer before the it fails. Retrograde intramuscularly pins, inserted via arthrotomy from the knee up into the shaft are an alternative option.
 |
| Intracondylar fracture fixed with sliding screw and plate |
In all cases it is imperative that the alignment of the knee is anatomical when finished. The lateral outer margin of the condyle makes a 95 degree angle with the transverse axis of the knee and a 95 deg.many fixed angle devices (such as the sliding screw shown here) make use of this for alignment. If the fixed screw or blade is positioned parallel with the knee's transverse axis anatomical alignment is assured. Intramuscularly devices and the modern "locking plates" lack this safeguard and the surgeon must be wary of varus or valgus malalignment.
Patellar Fractures
The patella can fracture as a result of a direct below, or it may fail directly, or aided by a pull, of the quadriceps. A direct blow will result in an intact quadriceps mechanism. The mechanism is often ruptured. Ask the patient to extend the knee against gravity. If he cannot do so the mechanism is not intact and surgery is indicated.
 |
| Patella fracture with ruptured quadriceps mechanism |
An X rays sign of a probable ruptured patella is a transverse fracture with more than 3 mm gap between the fragments. An direct blow may produce a vertical fracture. Do not be fooled by a bipartite patella. This is a bone in the quadriceps usually at the superior pole of the patella. Check the other side. A bipartite patella is often bilateral and has well rounded borders. It occurs in 1% of the population. It is sometimes the cause of knee pain.
Treatment
Undisplaced patella fractures can be treated conservatively. A "Stovepipe" plaster from groin to ankle, with knee in full extension is applied. Union takes about 6 weeks. Displaced transverse fractures will need surgery. The quadriceps mechanism has to be restored. A tension band is usually the best way to reduce the fracture and mend the quadriceps mechanism.
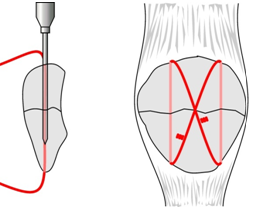 |
| Tension band for patella fracture. Two parallel K wires are placed along the axis of the knee and tensioned using a stainless steel wire crossed as a figure 8 over them |
Fractures or avulsions of the superior or distal pole also need surgical treatment. The quadriceps mechanism is not intact and may need direct suture. For patellar tendon ruptures, the suture line is protected by a thick stainless steel wire (threaded from a drill hole below the patellar tendon insertion on the tibia to above the patella.)
The quadriceps is a strong muscle and all internal fixations also need protection in a postoperative plaster cast.